Antimicrobial Resistance: a top 10 global health threat
The COVID-19 pandemic has only exacerbated the evolution of antimicrobial resistance
6 minute read
Antimicrobial resistance is when microbes: bacteria, viruses, fungi and parasites change over time and no longer respond to medicines that typically eradicate them. This ultimately makes infections harder to treat, and increases the risk of disease spread, illness, and death among populations. Antimicrobial resistance has been declared one of the top ten global health threats by the World Health Organization.
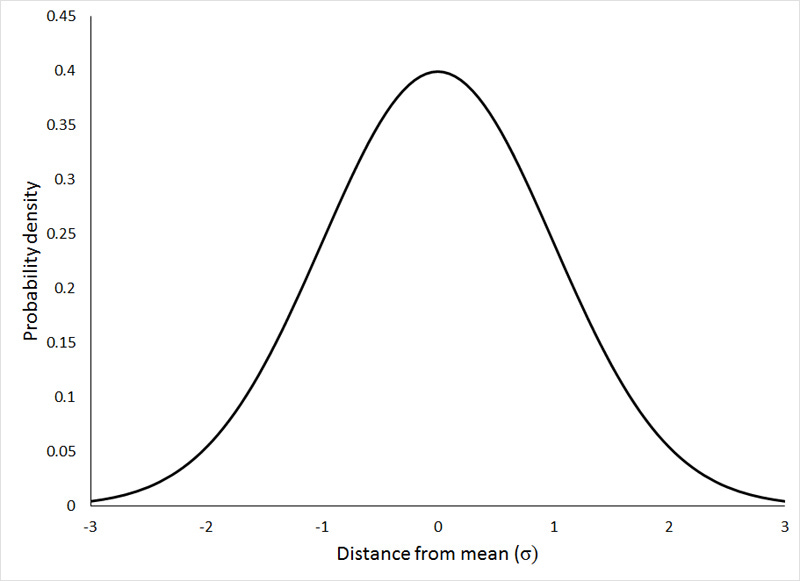
All populations exist in a normal distribution:
Where the majority of individuals within a population exist around the mean (average) and the extremes at both ends have fewer individuals.
In microbial populations, the same is true. If our X-axis represents susceptibility to an antimicrobial drug (a medication that will kill a given microorganism), there will be some organisms that will be killed very quickly (the left tail of the normal distribution). The majority of them will be killed under ‘normal’ circumstances (i.e. with a standard course of a given treatment), but then there will be some at the other extreme end that are more resistant to begin with, and will need longer treatment or higher concentrations of a given treatment to kill.
Antimicrobial resistance will occur naturally over time as a result of genetic changes within microbial populations (called microbial evolution). However, the main driver and accelerator of antimicrobial resistance is the misuse and overuse of antimicrobials. When we say overuse and misuse, we mean the following:
Keep reading with a 7-day free trial
Subscribe to Unbiased Science to keep reading this post and get 7 days of free access to the full post archives.